Virginia hospitals are monitoring painkiller prescriptions more closely and taking other steps to curb the opioid epidemic, and the efforts may be paying off: Drug overdoses in Virginia have dropped (slightly) for the first time in six years.
Virginia hospitals are monitoring painkiller prescriptions more closely and taking other steps to curb the opioid epidemic, and the efforts may be paying off: Drug overdoses in Virginia have dropped (slightly) for the first time in six years.
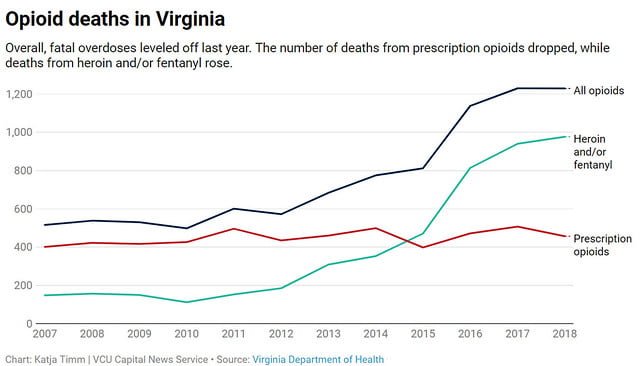
In 2016, the opioid epidemic was declared a public health emergency in Virginia. Fatal opioid overdoses increased steadily from 572 in 2012 to 1,230 in 2017. Last year, however, the number of deaths dipped, to 1,213, according to preliminary statistics released this week by the Virginia Department of Health.
The decrease coincided with data from the U.S. Centers for Disease Control and Prevention showing a decline in overall prescriptions of opioids — and with moves by Virginia officials and physicians to apply more scrutiny before issuing such prescriptions.
Dr. Charles Frazier, senior vice president at Riverside Health System in Newport News, said his medical practice and others across Virginia are prescribing narcotics in a more controlled and efficient way.
Frazier was involved in the creation of Virginia’s Emergency Department Care Coordination program.
Established by the General Assembly in 2017, the EDCC’s purpose is to “provide a single, statewide technology solution that connects all hospital emergency departments in the Commonwealth” for the purpose of extending and improving patient care, according to ConnectVirginia, a statewide health information exchange.
“The purpose of the EDCC is to integrate alerts,” Frazier said. “It shows us alerts of whether or not they (patients) have been in other emergency departments, information on how they were treated, with the idea being if a patient came in: Who is their primary care doctor? Who can we connect them to?”
Frazier said that in the program’s first phase, all hospitals in Virginia were required to submit a year or two of historical patient visit data to the EDCC information exchange by June 2017.
“The system is set up to alert emergency department providers and staff if the patient is a frequent emergency department patient, and also if they have been aggressive or abusive to staff,” Frazier said.
Frazier said that most of the time, the system is used to direct patients to proper care.
“I think part of the problem is if people have a hard time with transportation, they go to the ER for basic health care,” Frazier said. “If you go to the emergency room for a sore throat, for example, that can be expensive.”
The second phase of the EDCC, which was implemented last July, involves notifying primary care doctors if their patient is in the emergency department. If the system can identify a patient’s primary care doctor, it will send an alert.
“One thing we are starting to see are health systems collaborate on patients,” Frazier said. “There was a patient at Bon Secours who kept going to various emergency departments around Richmond — VCU, St. Francis, and others. With the EDCC program, they could see where they had been to, and the health systems worked together, along with the insurance company, to help the patient get the primary care they needed.”
Virginia’s Prescription Monitoring Program
Gov. Ralph Northam, a physician himself, helped create the EDCC. He also has been an advocate for the state’s Prescription Monitoring Program.
Under that program, Frazier explained, “Every time a pharmacy prescribes a controlled substance, they need to submit the information to the state — the duration, the dosage — and the system tracks how many times and how many providers have prescribed to the patient.”
Virginia Board of Medicine regulations require seeing chronic pain patients every 90 days and conducting drug screens to make sure patients are taking their medications and not taking illicit substances. Regulations also require prescribing an opioid antidote in certain high-risk situations.
“If you’re treating someone with higher dosages, the regulations outline preventative measures for overdose,” Frazier said.
Opioid overdose fatalities decline
Health officials’ concerns about opioids have grown as fatal overdoses spiked over the past decade. Preliminary numbers show that 1,484 people died from drug overdoses in Virginia in 2018. That is more deaths than from guns (1,036) and traffic accidents (958).
The total number of overdose fatalities was down slightly from 1,536 in 2017.
The vast majority of drug overdose deaths involve opioids. Of the 1,230 opioid-related fatalities last year, about 460 involved prescription medications and the rest involved heroin and/or fentanyl.
The number of prescription opioid deaths dropped from 507 in 2017 to 457 last year. On the other hand, deaths from heroin and/or fentanyl jumped from 940 to 977.
‘These numbers should give us some optimism’
In a press release, Attorney General Mark Herring thanked “advocates, families, doctors, recovery communities, elected officials, public health professionals and others who have helped reduce Virginia’s number of fatal drug overdoses for the first time in six years.”
Herring has been a strong advocate for fighting the opioid epidemic. He has taken a range of actions — from pushing to expand the Prescription Monitoring Program, to producing a documentary titled “Heroin: The Hardest Hit,” to suing Purdue Pharma, the creator of Oxycontin, on grounds that it helped create and prolong the opioid epidemic in Virginia.
“We should be heartened and hopeful to see that overdose deaths seem to have plateaued and may be starting to decline, but nearly 1,500 overdose deaths, mostly from opioids, is still a staggering number that shows this epidemic is far from over,” Herring said.
“But these numbers should give us some optimism that Virginia’s comprehensive approach — emphasizing treatment, education, and prevention, along with smart enforcement — can produce results and save lives.”
New controls on opioid prescriptions
Frazier said the biggest impact on the opioid epidemic might stem from rules imposed last year by the Virginia Board of Medicine.
“Across the state,” Frazier said, “we’ve seen a decrease in the number of opioid prescriptions and the duration of treatment for acute pain — a tremendous difference.”
Frazier said opioids sometimes are appropriate and sometimes aren’t.
“There are people who break their leg and need it for a few days, but for people who have chronic pain, they may require ongoing opioids for a long time,” he said. “While we first try non-opioid therapies, the reality is sometimes opioids are the most effective treatment for chronic pain.”
Patients can self-administer pain relief
When opioids are appropriate for treatment, health care professionals want to ensure that patients can receive their medication safely and easily. Virginia Commonwealth University Medical Center Hospitals have a specific technique allowing patients to self-administer drugs.
Samantha Morris, a care partner at the center’s Emergency Department, said narcotics can be administered directly to a patient, by the patient, with the press of a button. This involves a device called a patient-controlled analgesia pump.
“Fentanyl is usually what I see being prescribed the most, and that one is usually administered through a PCA pump,” Morris said. “It delivers some form of narcotic, usually fentanyl, and the patient presses a button to administer themselves a dose every five to ten minutes, depending on the drug.”
The amount of time a dosage from the PCA pump can be administered is based on the strength of the drug prescribed.
“I see patients mostly in the burn victim unit because they’re in a lot of pain,” Morris said.
Morris said she sees patients come in for opioid-related incidents all the time.
“It’s really difficult, because if a patient is addicted to any kind of substances, whether it’s amphetamines or any kind of narcotic to begin with, we can’t administer pain management, because it’s not going to affect the same pathway.”
By Katja Timm / Capital News Service