The adapter had to be small and light, measuring 22 millimeters in diameter on either end with a 4-millimeter hole running through it.
Mechanical engineering master’s student Genevieve Gural sketched out a rough design of the device with pen and paper while the rest of the team at the Design, Research, and Education for Additive Manufacturing Systems (DREAMS) Laboratory, led by mechanical engineering professor Chris Williams, batted around ideas for making it. They could 3D print it using filament extrusion, squeezing layers of hot plastic out to form the shape; or selective laser sinter it, building up layers of laser-melted plastic powder; or machine it, cutting away at stock material. Whatever they did, they had to be quick.
Days before, earlier in March, when leaders in Carilion Clinic’s pulmonology division spoke with Williams about the supplies they would need to fight COVID-19 locally, the Carilion team brought up the adapters. If intensive care units were to experience a surge of COVID-19 patients, the influx could overwhelm their existing supply of ventilators. To prepare for that scenario, the team aimed to repurpose the hospital’s fleet of bilevel positive airway pressure, or BiPAP, machines — typically used to help people with sleep apnea breathe evenly at night — as low-level ventilators. The adapters played into the modified setup they had in mind for the machines.
Led by Edmundo Rubio, Carilion’s chief of pulmonology and critical care medicine and a professor at the Virginia Tech Carilion School of Medicine, the staff worked out a setup that would involve a BiPAP machine delivering oxygen to an intubated patient. As the patient exhaled, that breath and the virus particles it carried would exit through an exhalation port that branched from the tubing. The staff would attach the adapter to the port, and to the adapter, they would attach a standard filter to trap virus particles, preventing them from escaping into the room.
They had initially assembled an adapter with parts on hand, fixing 22-millimeter connectors onto both ends of a 4-millimeter connector. The three-piece device did the trick, with the latter part doing extra work to slow exhaled air flow out of the filter. But it would be problematic to assemble more devices that way. Each time, they would have to pull the parts from multiple sterilized kits and throw out other valuable components. Using three different parts to assemble the device also lent to tiny cracks — and the risk of leaking the virus.
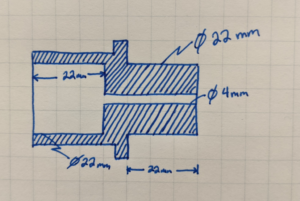
The DREAMS team’s task was to combine the three parts into one and produce many more Carilion-approved, streamlined adapters in a few weeks, for use in BiPAP ventilation along with other forms of oxygen therapy. Graduate students Lindsey Bezek, Bemnet Molla, Sam Pratt, and Gural broke off onto parallel manufacturing paths to try filament extrusion printing, selective laser sintering, and machining the device. In this case, machining gave the device a smoother seal and faster production — it would take about two to three minutes to make each one. The team headed down that path.

Less than a week after the project began, Pratt dropped off a test set of adapters for Carilion staff. They requested 200 adapters. As the design went through infection safety and regulatory review, Williams tapped mechanical engineering professor Wing Ng and his local company, Techsburg, to prepare to batch produce the devices.
This process, equal parts speed and scientific integrity, carried out in swift loops of design, revisions, medical feedback, and patient safety reviews to finalize products and prepare for larger-scale production, has defined how a group of more than 75 Virginia Tech faculty, students, and staff have worked to respond to COVID-19 over the past month.
In mid-March, the interdisciplinary group split into teams to carry out 10 projects in rapid science and production, working together to provide Southwest Virginia medical professionals with personal protective equipment and ventilation supplies, and the insights to inform their use.
The group unites experts in subjects like product design, fabrication, materials science, biosciences, virology, and sterilization, from such colleges and institutes as the College of Engineering, the College of Science, the Virginia Tech Carilion School of Medicine, the Fralin Biomedical Research Institute at VTC, the School of Architecture + Design, and University Libraries. The group also worked with the Edward Via College of Osteopathic Medicine.
“We’re all trying to do our best to respond,” said Williams, who has helped organize the effort. “We needed some way to pull everyone’s resources, expertise, and capabilities together. Through campus-wide coordination, we can leverage all of our resources and standardize the solutions distributed to ensure their widespread adoption, their integrity, and their safe deployment and use in health care.”

Pooling perspectives in engineering design, science, and medicine
The group’s projects are driven by requests and ideas from members of the local medical community, like Rubio. In search of engineers that could design and produce modifications for the BiPAP machines, Rubio reached out to Michael Friedlander, vice president for health sciences and technology at Virginia Tech and executive director of the Fralin Biomedical Research Institute. Friedlander connected him with Virginia Tech engineering researchers like Williams and Joseph Meadows, a professor in the Department of Mechanical Engineering.
“Across the university, we’re seeing researchers from a variety of fields quickly shift their focus to join these COVID-19 response efforts,” Friedlander said. “It has been important to connect our colleagues at Carilion Clinic, who can relay their clinical expertise and firsthand experience with treating these patients, with our research faculty, who have been working around the clock to address clinical needs. The world is looking to science right now to address the pressing global health challenge, and it is humbling to see our Hokie community rising to the occasion.”
Meadows is now leading the design of a key upgrade for the BiPAP machines: flow meters, in-line sensors to measure air flow to the patient in real time, enabling doctors to calibrate settings for individual scenarios. Rubio explained that with modifications like flow meters, the machines can relieve pressure on traditional ventilators as staff treat COVID-19 patients.
“Carilion Clinic has gone to great lengths to prepare for a surge of patients, and right now, ventilators are well in hand, but if that surge occurs and overwhelms our current ventilator capacity, these BiPAP S/T systems will allow us to support patients with less severe disease or those that are beginning to improve and need less ventilatory support,” said Rubio.

3D printing and laser cutting face shields
Along with their work on ventilator components, the group aims to supply personal protective equipment in projects that range from the DREAMS lab’s first steps toward 3D-printed mask production to the forthcoming rollout of 3D-printed and laser-cut face shields, which can provide healthcare workers with a first line of defense.
A team led by mechanical engineering professor Alex Leonessa, director of the Terrestrial Robotic Engineering and Controls Laboratory, and Liam Chapin of the Field and Space Experimental Robotics (FASER) Laboratory, headed by mechanical engineering professor Erik Komendera, is organizing the mass production of face shields after rapidly prototyping and running 15 designs by staff from Carilion Clinic and LewisGale Hospital.
“We’ve considered the technical challenges in terms of making production feasible, assembly quick, and sterilization and disposal easy to carry out responsibly,” said Leonessa. “In a way, that’s what we train our students to do throughout the curriculum. Students learn to assess the needs of the user, come up with a conceptual design that fits those needs, and when that is verified, create a final design. It’s an engineering feat, and they’re more than prepared to do it.”
With infection control approval on a single, finalized face shield design, the team is ramping up production. They now aim to recruit volunteers with the at-home capacity and resources to 3D print, laser cut, and safely contribute parts for the face shields.
Chapin, an undergraduate engineering student, said he’s witnessed an outpouring of support from the student body, among both those in the lab and those who’ve contacted him to offer help. “I am proud to be a part of this effort, proud to have risen to the challenge along with my teammates, and proud to be doing my utmost to keep people safe,” said Chapin. Gural summed up the sense of teamwork and determination among graduate students in a word: “awesome.”
“At a time when our commitment to community, resilience, and service is more important than ever, I am so proud to see our students and faculty stay true to those values,” echoedJulia Ross, dean of the College of Engineering.

Rapid science to inform rapid design and production
As teams standardize designs and plan the next steps in production, others examine how the response will uphold patient safety as supplies are delivered to hospitals, as well as the efficacy of different kinds of personal personal protective equipment in filtering particles.
Linsey Marr, the Charles P. Lunsford Professor of Civil and Environmental Engineering, is conducting ongoing experiments to test the efficacy of N95 respirators after they’ve gone through various sterilization techniques. Marr and her graduate students are evaluating how well the respirators retain their efficacy in filtering particles following sterilization with techniques including ethylene oxide, a method requested for testing by leadership at Carilion Clinic, and hydrogen peroxide vapor.
Marr is also testing the efficacy of alternative mask materials available off the shelf, like the Hanes Beefy-T, felt, Shop-Vac bags, HVAC filters, auto rags, and microfiber cloth. Matt Hull, Marr’s colleague on the NanoEarth Team at the Institute for Critical Technology and Applied Science, coordinated collection and safe distribution of materials to her lab for testing.

“I think Linsey is a lynchpin in this,” said Williams, who has also sent Marr leading 3D-printed mask designs for evaluation, including the first FDA-approved 3D-printed mask. If the latter passes her tests, his team will move to produce them en masse. The DREAMS lab may also work on a novel mask design of its own, if needed.
“Without Linsey’s lab, we would be relying on our best engineering guess,” Williams said. “Their unique capabilities will enable us to make some very quick quantitative assessments of the efficacy of these alternative PPE solutions.”
Once the rapid production projects clear patient safety and regulatory reviews and the steps of mass production for approved designs, assembly, and delivery of supplies to area hospitals have begun, the designs will be posted online in an open-source format for broader use.
“For everyone involved, the fundamental thing we have in common is that we just want to help,” said Williams. “The Ut Prosim motto is embedded in all Virginia Tech faculty, staff, and the student body. I think it really shines here.”
– Written by Suzanne Irby. Whitney Slightham and Eleanor Nelsen contributed reporting.



